You worked hard to get through med school and specialty training, and you like to think it’s all paying off in increased earnings because of your credentials. You’re genuinely concerned for your patients, and take pride in providing the best cardiovascular care available. You can’t imagine why anyone would opt to receive the same services from another provider who doesn’t have the same c.v, especially when patients don’t set payer rates, so why would you think you should settle for anything less out of your billing service?
Medical Billing Blog
Barry Shatzman
Recent Posts
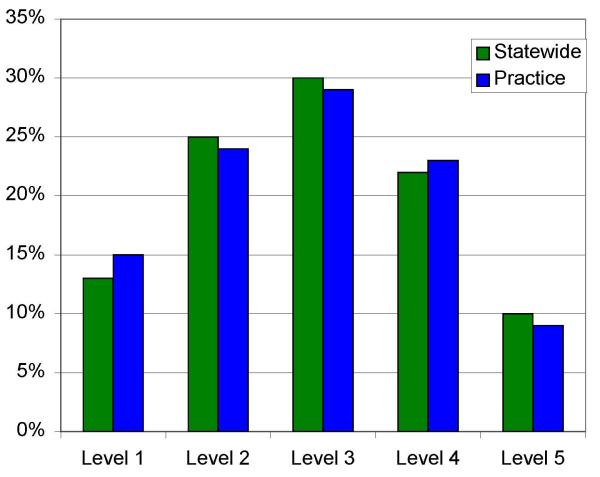
78% Revenue Increase Due To Certified Cardiology Coding
Omnibus Rule Bridges Gap Between HIPAA & HITECH
On Jan. 25, 2013, the Department of Health and Human Services (HHS) published the “Omnibus Rule,” which is a final set of regulations that enforces various provisions of Health Information Technology for Economic and Clinical Health (HITECH) Act which in turn is designed to enhance the Health Insurance Portability and Accountability Act (HIPAA). In general, the new rules expand the obligations of physicians and other health care providers to protect patients’ protected health information (PHI), extend these obligations to who has access to PHI, and increase the penalties for violations.
There are basic areas providers will need to comply with:
CPR For Your ICD-10 Transition: Check, Prepare, Respond
The healthcare industry is changing rapidly and providers are facing many new challenges, with ICD-10, meaningful use, and fee schedule reductions being only a few. If you feel like there are just too many cats in the herd, there is one area where you can take control of the situation, and that is by re-evaluating the effectiveness and adaptability of your billing function. Whether you have an in-house billing staff, or an outsourced revenue cycle management team, it’s crucial to make an accurate assessment of the processes associated with your billing function to ensure that you are not part of the majority of practices expected to face serious cash flow problems when ICD-10 goes into effect next October.
Medical Providers Can Look To Canada For Lessons In ICD-10
When the transition to ICD-10 officially begins on October 1, 2014, those in the US healthcare industry will be in a position to benefit greatly from lessons learned by our neighbors inCanada, who also recently made the transition between 2001 and 2004. Canadians already experienced similar transition situations to what the United States will be facing according to Cindy Grant, Certified Healthcare Information Manager (CHIM) and ICD-10 practice lead at TELUS Health Solutions in Toronto,Ontario; and Kerry Johnson, MAEd, CHIM, senior lecturer and HIM instructional coordinator at the University of Ontario, Institute of Technology in Oshawa,Ontario. Coders in Canada struggled most with anatomy and physiology, not the coding logic itself. "It wasn't so much the coding system and how the codes work," says Johnson. "We found them struggling with anatomy and physiology and understanding what exactly the intervention was, including determining the root operation."
A recent survey conducted by the Workgroup for Electronic Data Interchange (WEDI) regarding the preparations for transitioning to ICD-10 being conducted by healthcare providers shows that nearly half of the survey group either have not started preparing for ICD-10 or do not know when they expect to start their testing.
Managing a successful medical practice involves more than just practicing medicine. You must also view it as a successful business, and put into place sound business practices, as well. Many providers are seeing their revenues decline as payers are reducing fee schedules, so it’s more important than ever to collect every dollar that you’re entitled to, and to manage how you budget that revenue to keep your practice running in the black.
HIPAA and HITECH Evolution Responds To Technological Advances
The HITECH Act (Health Information Technology for Economic and Clinical Health) was passed in February 2009 as part of the American Recovery and Reinvestment Act, it expanded the obligations of covered entities and business associates to protect the confidentiality and security of Protected Health Information (PHI). Passage of the HITECH Act was timely because its main purpose was to address voids inherent in HIPAA due to the development of new technologies that did not exist at the time HIPAA was originally implemented.
Revised Warnings For Docs Using Cloned Notes
As a follow up to my recent post “Avoiding Payment Denials for Cloned Notes,” the Centers for Medicare & Medicaid Services (CMS) has issued new instructions to Medicare Administrative Contractors (MAC’s), Recovery Audit Contractors (RAC’s), and Zone Program Integrity Contractors (ZPIC’s) to look for claims generated from Electronic Health Records (EHR’s) that do not contain adequate information.
Medicare Administrative Contractors (MACs) warn that individualized patient notes are required for each patient visit, and that use of “cloned notes” may cause a provider to overlook new information, resulting in treatment, safety, and quality issues.
Use Better Collection Techniques To Increase Patient Payments
It is said that “a bird in the hand is worth two in the bush,” and that is especially true when you’re talking about collecting payments from patients at the time of service. According to the AMA, the average cost to physicians for collecting monies owed and processing claims is 10 – 14 percent of gross revenue, butthere are ways to be more efficient, reduce these costs, and collect payments faster. The AMA website offers a Point-of-Care Pricing Toolkit to help you collect payment from patients before they walk out the door.