According to several Congressional leaders, preventing a 21% cut in Medicare Physician Fee Schedule payments in 2015 under the flawed Sustainable Growth Rate (SGR) formula remains the top healthcare priority for Congress this year. The latest SGR cut is scheduled to take effect when the current short-term patch expires at midnight on March 31st.
Medical Billing Blog
SGR is the Top Healthcare Issue for Congress in 2015
The United States Senate has joined the House of Representatives and passed legislation to prevent a 24% cut in physician fee schedule payments from occurring today as previously scheduled. Instead, Medicare physician fee schedule payments will continue to be paid as they have been for the past 3 months. Although the legislation must be signed by the President in order to become effective, the President has indicated that he will sign this legislation once it reaches his desk.
Yesterday, by a voice vote, the House of Representatives passed legislation postponing the 24% physician fee schedule cut slated to take effect on April 1, 2014. However, the legislation went well beyond just temporarily fixing the SGR problem, it also made a number of other changes that will have long-lasting implications. A listing of those changes is at the end of this message.
Permanent 'Doc Fix' May Be On Hold As House Passes Short-Term Patch
MARY AGNES CAREY: Welcome to Health on the Hill. I’m Mary Agnes Carey.
On February 6, the House Ways and Means Committee, House Energy and Commerce Committee, and Senate Finance Committee introduced a bi-partisan/bi-cameral bill to repeal the Medicare Sustainable Growth Rate (SGR) effective April 1, 2014. H.R. 4015. The Medicare Provider Payment Modernization Act consolidates three previously passed bills by each committee into a single framework to repeal and replace the flawed SGR.
Update: Sustainable Growth Rate (SGR) Reform
On Thursday afternoon (2/6) the House Ways and Means Committee, House Energy and Commerce Committee, and Senate Finance Committee leadership introduced a bi-partisan/bi-cameral bill to repeal and replace the Medicare Sustainable Growth Rate (SGR) formula. The Congressional sponsors have provided a section-by-section summary for your review.
City of Detroit and Retirees Reach Agreement on Health Insurance
The city of Detroit and its retirees have reached an agreement in a health insurance dispute that may end a lawsuit against the city. Retirees filed suit in November to stop the city from shifting them to Medicare and giving those under age 65 a $125 monthly stipend to buy their own insurance. The parties reached an agreement in principle Thursday night covering benefits through the end of 2014, mediators in Detroit's bankruptcy said Friday in a statement. Some features of the deal include the increase to $300 in the monthly stipend for retirees over age 65 who aren't eligible for Medicare. The stipend for retirees under age 65 will be increased to $175 if the household income is less than $75,000 and the retiree acquires insurance under a health care exchange. The stipend is $50 more than the amount proposed last year by emergency manager Kevyn Orr. A lawsuit retiree groups filed in bankruptcy court Jan. 9 challenging the city’s plan to slash benefits will be dismissed as a result of the settlement, according to a statement from the Detroit bankruptcy court mediators.
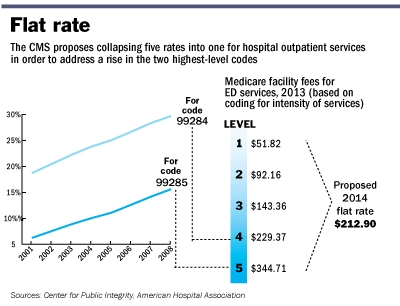
CMS issues 2014 Outpatient Facility Policy and Payment Changes
Last November, CMS released a final CY 2014 hospital outpatient and ambulatory surgical center (ASC) payment Final Rule. Most significantly, “CMS will replace the current five levels of hospital clinic visit codes for both new and established patients with a single code describing all outpatient clinic visits.” CMS believes that a single code and payment is administratively simpler for hospitals and “better reflects hospital resources involved in supporting an outpatient visit.”
Centers for Medicare and Medicaid Services (CMS) released its 2014 Medicare physician fee schedule (PFS) Final Rule. CMS calculates the 2014 Physician Fee Schedule Conversion Factor (CF) to be $27.2006, or a 20.1% reduction from the current CF of $34.0230. Total payments under the fee schedule in 2014 are projected to be at $87 billion, according to CMS. Payments to physicians are calculated primarily on three key factors: the resource-based relative value scale (RBRVS), the geographic practice cost indexes (GPCIs), and the monetary conversion factor (CF).
MBR Explains: Quality Improvements - Key Features of the Affordable Care Act by Year -- 2010
Continuing our series on the key features of the Affordable Care Act, we will now look into the changes that took effect in 2010 that sought to improve quality and lower cost of healthcare. As previously mentioned, the Patient Protection and Affordable Care Act was signed by President Obama on March 23, 2010. The law aims to increase the quality and affordability of health insurance, lower the uninsured rate, and reduce the costs of healthcare for individuals and the government. However, a number of the mechanisms – mandates, subsidies, and insurance exchanges – are to be rolled out over four years and beyond. Below is an overview of some of the key quality improvement provisions that took effect in 2010.